When it comes to understanding the complexities of the human brain, recent findings on split-brain communication present fascinating insights. A surprising statistic reveals that just a few fibers are critical for communication between the two hemispheres of the brain. This capability, discovered in a groundbreaking study, illustrates the remarkable adaptability and resilience of our neurological functions. By diving deeper into the concept of split-brain communication, we can appreciate how minimal connections can sustain cognitive functionality, providing significant implications for rehabilitation and healing strategies following brain injuries.
The Science Behind Split-Brain Communication
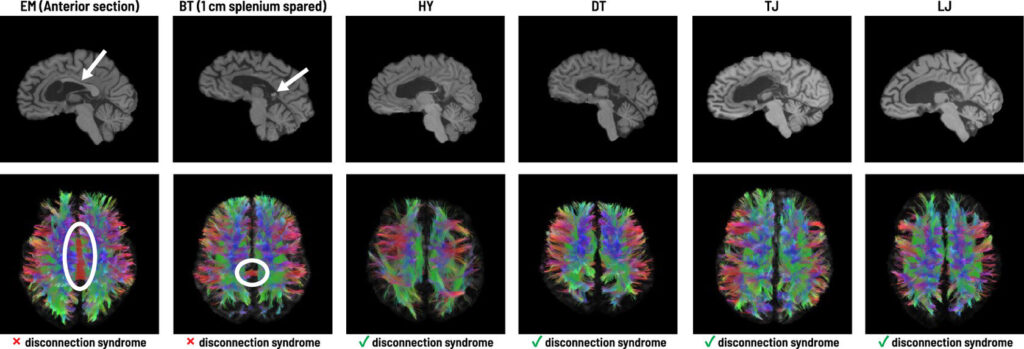
The study, led by a team from the University of California and the University of Cologne, highlights that only a few fibers from the corpus callosum—the largest fiber bundle in the brain—are necessary to maintain interhemispheric communication. Their research, documented in the _Proceedings of the National Academy of Sciences_, challenges previous beliefs that significant damage to this critical bundle inevitably leads to impairments in speech, motor skills, and perception.
By utilizing functional magnetic resonance imaging (fMRI), the team analyzed how varying extents of corpus callosum damage influenced neural synchronization. Remarkably, while complete transection resulted in a stark reduction of communications, those with preserved fibers revealed nearly normal interhemispheric exchange. This demonstrates that even minimal connections are sufficient for the brain’s complex network architecture to function effectively.
Implications for Understanding Brain Plasticity
The implications of these findings extend far beyond academic curiosity. The adaptability showcased in split-brain communication provides crucial insights for rehabilitation practices. Following incidents like strokes or traumatic brain injuries, when significant parts of the brain may be damaged, the potential for recovery largely hinges on the brain’s neuroplasticity.
As explored in our analyses of high salt diets and brain inflammation, understanding how the brain can reorganize is essential for creating targeted therapeutic interventions. For patients with damaged communication pathways, rehabilitation efforts should focus on enhancing the remaining connections, utilizing exercises that stimulate the brain’s capacity to adapt and compensate for lost functions.
Cognitive Functions and Location-based Impacts
Interestingly, cognitive functions are significantly influenced by the location of brain activity. A study published by our research team at brain health locations details how geographical discrepancies affect neural pathways and functions. The adaptability of the brain observed in split-brain communication is a profound indicator of how location and environment can contribute to cognitive abilities and recovery processes.
By understanding these influences, healthcare professionals can better tailor therapeutic strategies that harness the brain’s natural abilities for recovery and improvement.
Artificial Intelligence’s Role in Therapeutics
Moreover, split-brain communication research correlates with ongoing discussions about artificial intelligence within healthcare. Tools that analyze neural data can enhance understanding of brain functions and improve patient outcomes post-injury. As discussed in our article on AI in health care, the integration of advanced technological strategies may revolutionize rehabilitation practices by providing insights into the brain’s functional networks.
The perspective gained from split-brain research can complement these technological advancements, shaping future healthcare policies to create innovative rehabilitative approaches that tap into both human adaptability and machine efficiency.
Long-term Effects of Brain Injuries
The understanding of split-brain communication also plays a vital role in comprehending the long-term impacts of brain injuries, particularly in conditions such as Long COVID. Recent findings point to brain inflammation leading to severe cognitive disruptions, all of which benefit from research insights into how limited interhemispheric communication can sustain cognitive processes. For those interested, our detailed study on Long COVID and brain inflammation elaborates on how these connections affect overall brain health.
Furthermore, recognizing the critical importance of preserving brain function through disconnection syndromes can guide future therapeutic endeavors, which are essential for sustaining quality of life after such health challenges.
Conclusion: The Future of Neurorehabilitation
In conclusion, the findings associated with split-brain communication present a new paradigm in our understanding of brain functionality and rehabilitation possibilities. As we continue to delve into the intricate mechanisms of brain communication, it becomes increasingly apparent that even partial connections can retain complex cognitive functions. The interplay between structure and function within the brain remains a promising area for therapeutic interventions aimed at recovery and rehabilitation.
To deepen this topic, check our detailed analyses on Medical Innovations section.